- Spot checks miss the full picture of hypertension: HBPM and office readings provide limited snapshots. They don’t capture 24-hour averages, nighttime blood pressure, dipping status or true variability –– the factors that directly influence cardiovascular risk and clinical decision-making.
- ABPM is clinically superior, but operationally limited: ABPM is a Class 1A guideline-recommended tool and the only way to fully assess circadian blood pressure patterns. However, workflow burden, device scarcity, patient discomfort and logistical barriers prevent widespread use.
- Hypertension care needs scalable cuffless ABPM: We know 24-hour data improves diagnosis and outcomes, yet most patients never access ABPM screening. Improving diagnosis requires delivering ABPM-level insight in a more accessible, patient-friendly and scalable format.
On a daily basis, a common scenario occurs in thousands of medical appointments across the United States. A well-meaning physician advises a patient with borderline to high blood pressure to purchase a home blood pressure monitor (HBPM) and record the reading twice a day for a week.
Even among the most compliant patients who bring their results to a follow-up visit, the hypertension (HTN) picture remains incomplete. HBPM doesn’t provide 24-hour average blood pressure readings, unlike ambulatory blood pressure monitors (ABPM). Spot readings don’t capture blood pressure changes at night, during exercise, while eating, when stressed and during mood swings.
Meanwhile, HTN remains the most common cardiovascular disease worldwide. One in four patients still has uncontrolled blood pressure. Improving outcomes starts with better detection through accurate blood pressure measurement.
Why blood pressure spot checks aren’t enough
Blood pressure is dynamic, changing with activity, stress, sleep and medication timing. A single in-office reading and even spot checks at home don’t tell a full story. As guidelines increasingly emphasize out-of-office measurement, physicians face a practical decision about whether to recommend ABPM or HBPM.
Both tools have value, but they’re not interchangeable. And neither is a practical option to recommend at scale.
What is ambulatory blood pressure monitoring?
ABPM is a 24-hour monitoring cuff that automatically measures blood pressure every 15 to 30 minutes during the day and night. It provides daytime, nighttime and 24-hour averages.
The American College of Cardiology/American Heart Association 2017 Hypertension Guidelines recognize ABPM as a Class 1A recommendation for confirming hypertension. Only with 24 hours of readings can physicians accurately and confidently capture what office measurements cannot:
- Variability: Clinical decisions are based on averages, not single readings.
- Nighttime blood pressure: Nocturnal blood pressure is a critical predictor of cardiovascular morbidity and mortality. Without 24-hour monitoring, clinicians can’t assess dipping status or morning surge.
The average blood pressure over 24 hours allows physicians to distinguish between elevated in-office readings due to white coat syndrome and actual hypertension.
The limitations of cuff-based ABPM
Despite its clinical value, traditional cuff-based ABPM comes with both operational and patient-level challenges. This means few patients have access to 24-hour ABPM. According to a 2023 review of ABPM and HBPM in Hypertension Research, “Despite US guidelines supporting ABPM, ABPM is not widely available in the U.S. and is not commonly used in clinical practice.”
- Cuff-based devices are limited in most clinics.
- Patients must come in for a fitting and return the device the next day
- Cuff inflation every 15 minutes can cause discomfort, sleep disturbance, and behavioral changes
- Some patients remove the device prematurely
- Cuff inflation itself may raise systolic blood pressure by 11 to 20 mmHg in some individuals, complicating interpretation
- Devices require sterilization and workflow coordination before reuse
In short, a 24-hour ABPM test is clinically powerful, albeit impractical at scale due to operational burdens. Hypertension diagnosis with ABPM is only scalable with a cuffless ABPM option.
What is home blood pressure monitoring (HBPM)?
The limitations of ABPM lead many physicians to instead recommend HBPM for hypertension diagnosis and treatment. HBPM requires a patient to self-measure at home using a cuff device, typically twice daily over several days. Readings are logged manually or transmitted digitally.
HBPM’s wide accessibility makes it frequently recommended for ongoing monitoring.
Advantages of HBPM
- Accessibility: Cuff devices are widely available and relatively affordable.
- Patient engagement: HBPM encourages patients to participate in their health outcomes actively.
- Practical for medication titration: Multiple readings over days can inform treatment adjustments.
Limitations of HBPM
Compared to ABPM, HBPM has obvious limitations.
- It can’t capture nighttime blood pressure
- It depends entirely on patient adherence
- Improper cuff size, positioning errors and selective reporting can affect reliability
- Patients can freeze or even tense up when the cuff activates, affecting the reading
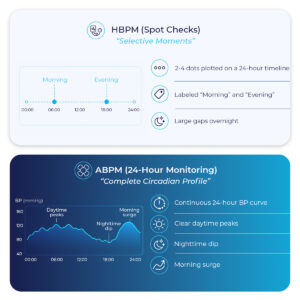
The core difference between ABPM vs. HBPM is simple: ABPM measures blood pressure across a full circadian cycle. HBPM measures selected moments chosen by the patient.

Cost and operational realities
ABPM that’s covered by insurance is reasonably priced. HBPM devices are also reasonable for patients to purchase and don’t require professional device turnover.
However, ABPM comes with high operational costs, including:
- Staff time for fitting and education appointments
- Device retrieval and manually uploading data
- Cleaning and preparation for the next patient
Even if ABPM was operationally easy to use, most clinics typically have limited devices, so real-world access lags behind recommendations.
HTN diagnosis in its current form in the U.S. presents a paradox for every cardiologist and primary care provider:
- We know 24-hour data improves diagnosis
- We know nighttime blood pressure predicts outcomes
- Yet most patients never access an ABPM
Better hypertension diagnostics with Cuffless ABPM
Scaling hypertension diagnosis and monitoring requires delivering the strengths of ABPM, while reducing patient burden and operational friction.
Biobeat’s wearable, cuffless 24-hour technology is the first FDA-cleared device to address the limitations of both ABPM and HBPM by:
- Eliminating repeated cuff inflation
- Improving comfort and compliance
- Expanding scalability beyond limited device inventories
- Enabling real-world phenotyping across day and night
For clinicians, this isn’t simply more data. Cuffless ABPM is a way to gather accurate averages on every patient who presents with indicators of HTN.
The question is not whether ABPM vs. HBPM is a better hypertension measurement tool. The question is how to offer 24-hour monitoring that’s patient-friendly and accurate enough to close the gap in hypertension control.
To schedule a demo of how Biobeat works or to learn more about how Biobeat’s cuffless Blood Pressure monitors can help improve HTN diagnostics and treatment, contact: info@bio-beat.com.